Reproduced with kind permission. This article originally appeared in the NADA Advocate eMagazine, published in December 2021. Readers can subscribe to the Advocate here.
Some people who use or are dependent on AOD can feel self-stigma—negative and internalised self-judgements resulting in shame, worthlessness and self-blame. For those people seeking support for their AOD use, this self-stigma can negatively impact self-agency, quality of life, access to services and participation in treatment.
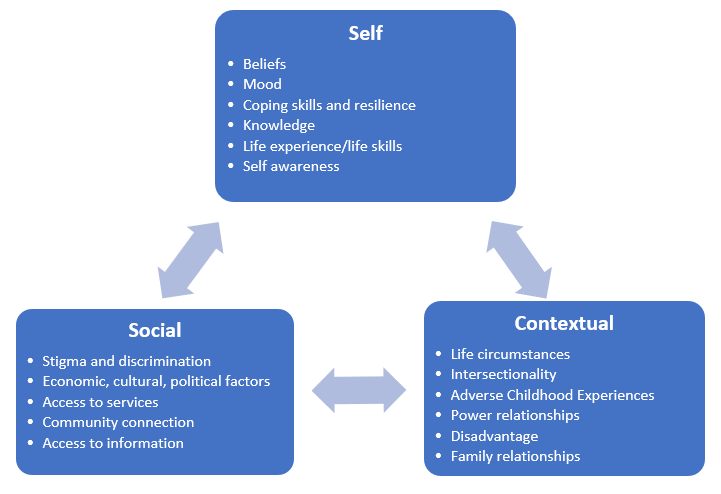
Self-stigma is a result of complex interactions between social, contextual and self-factors.[1] The framework below identifies these complex interacting factors which influence the development and perpetuation of self-stigma (click to enlarge).
 There is a link between shame and substance dependence,[2] however the understanding of its impact on recovery is limited. While shame can be a hindrance to recovery, it has also been found that addressing shame may also enhance recovery.[3]
There is a link between shame and substance dependence,[2] however the understanding of its impact on recovery is limited. While shame can be a hindrance to recovery, it has also been found that addressing shame may also enhance recovery.[3]What is shame?
Dr Brené Brown has researched shame and vulnerability for over 25 years using grounded theory methodology. She describes shame as 'the intensely painful feeling that we are unworthy of connection, love and belonging.'[4]
Dr Gabor Mate has spoken many times on the subject of shame, particularly as it relates to AOD use and dependence. He describes shame as a loss of contact with the self. People experiencing shame may believe, 'I am not good enough. There's something wrong with me.'
Shame feelings can be associated with low self-esteem, hostility, and psychological distress.[5] Someone dealing with shame might also feel:
- inferiority
- humiliation
- remorse
- embarrassment
- inadequacy
- unworthiness
- powerlessness.
These feelings in turn, can result in withdrawal from others and/or aggression, in an attempt to deflect feelings of shame.
Shifting from shame back to self
How can AOD workers support consumers who experience shame?
- Understand and acknowledge shame and how it presents—secrecy and silence encourage shame
- Support consumers to view themselves as more than their past behaviour
- Use a strengths based approach
- Show empathy and non-judgement—empathy is the antidote to shame
- Use non stigmatising language[6]
- Support consumers to overcome negative thoughts and beliefs by using motivational interviewing and cognitive behavioral therapy techniques that identify and modify unhelpful thinking patterns, underlying assumptions and thoughts about the self, the world and the future.
- Employ and support peer workers who have a lived experience
Ensure your practice and service is trauma informed by committing to the six core trauma-informed principles:- safety—emotional as well as physical e.g., is the environment welcoming?
- trust—is the service sensitive to people's needs?
- choice—do you provide opportunity for choice?
- collaboration—do you communicate a sense of 'doing with' rather than 'doing to'?
- empowerment—is empowering people a key focus?
- respect for diversity—do you respect diversity in all its forms?[7]
Resources
Providing trauma-informed care: a case study of Weave Youth and Community Services
This video explains trauma-informed care and the importance of personalised support when delivering this care.
Brené Brown's TED Talk 'Listening to shame' https://www.ted.com/talks/brene_brown_listening_to_shame.
The difference between empathy and sympathy
https://www.youtube.com/watch?time_continue=162&v=1Evwgu369Jw
Language matters
https://nada.org.au/resources/language-matters
[1] Adapted using concepts from Morrison (2006)
[2] Potter-Efron, R. (1987). Shame and guilt: Definitions, processes and treatment issues with AOD clients. Alcoholism Treatment Quarterly, 4(2), 7–24.
[3] Luoma, J.B., Kohlenberg, B.S., Hayes, S.C., & Fletcher, L. (2012). Slow and steady wins the race: A randomized clinical trial of acceptance and commitment therapy targeting shame in substance use disorders. Journal of Consulting and Clinical Psychology, 80 (1), 43-53.
[4] https://www.ted.com/talks/brene_brown_listening_to_shame
[5] Patrizia Velotti, Carlo Garofalo, Federica Bottazzi & Vincenzo Caretti (2017) Faces of Shame: Implications for Self-Esteem, Emotion Regulation, Aggression, and Well-Being, The Journal of Psychology, 151:2, 171-184.
[6] https://nada.org.au/resources/language-matters/
[7] Blue Knot Foundation
https://www.health.nsw.gov.au/mentalhealth/psychosocial/principles/Pages/trauma-informed.aspx
